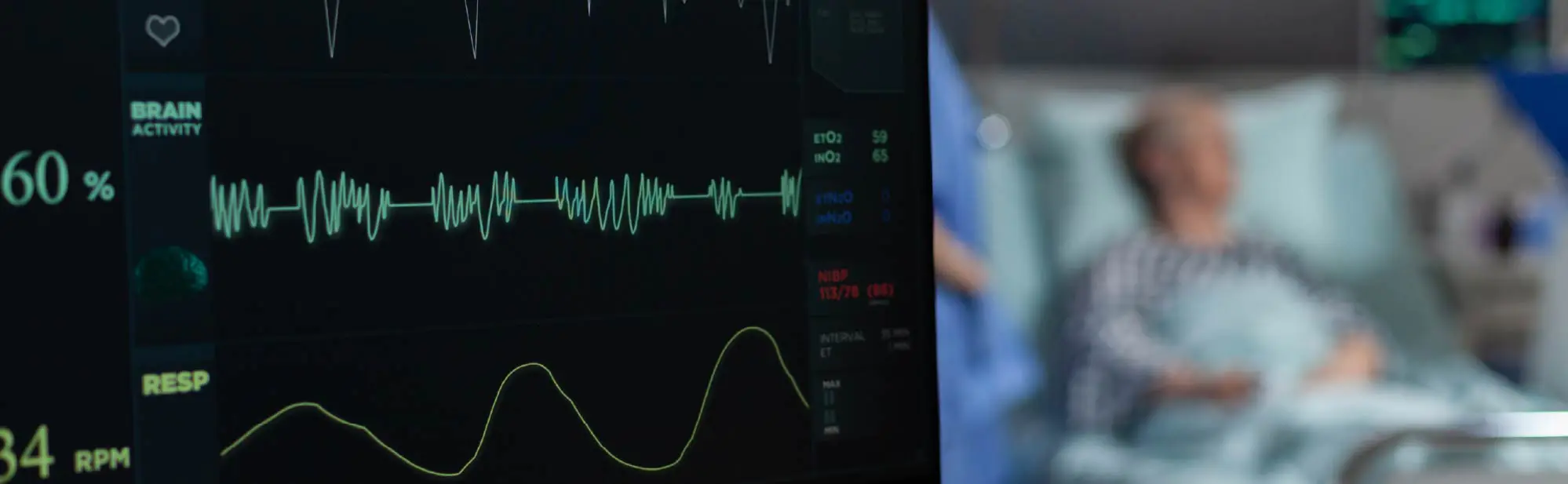
The patient monitor in the intensive care unit is a basic element of the life support system. Its task is to provide continuous, accurate and clinically interpretable monitoring of vital signs in patients with critical organ and system dysfunction.
Unlike monitors for general departments, intensive care systems must support invasive blood pressure measurements, advanced ECG analysis, capnography, monitoring of patients on mechanical ventilation (MVL), as well as stable operation in 24/7 mode without loss of signal accuracy.
Choosing a monitor for intensive care is an assessment not only of the list of parameters, but also of the system architecture, its modularity, reliability, integration capabilities and compliance with clinical scenarios of a particular department
In the intensive care unit, the patient monitor must provide continuous monitoring of parameters reflecting the state of the cardiovascular, respiratory and thermoregulatory systems. The choice of configuration should correspond to the profile of the department (general intensive care, cardiac resuscitation, postoperative ICU, etc.).
1.1. Electrocardiography (ECG)
ECG is the basic tool for assessing the electrical activity of the heart in conditions of hemodynamic instability.
For ICU, the monitor should provide:
3- or 5-leads (minimum)
Continuous calculation of heart rate
Automatic analysis of arrhythmias (asystole, ventricular tachycardia, ventricular fibrillation, bradycardia)
ST segment analysis (preferably in 5-leads)
In cardiac resuscitation, it is advisable to support 12-leads for diagnostic analysis of ischemic changes.
1.2. Non-invasive blood pressure (NIBP)
Non-invasive pressure measurement is used for initial monitoring and in stable patients.
The monitor must support:
Oscillometric measurement method
Modes: manual, automatic with interval, STAT
Display of systolic (SYS), diastolic (DIA) and mean arterial pressure (MAP)
Profiles: adult / pediatric / neonatal
In critical patients, NIBP does not replace invasive monitoring, but is used as an additional (baseline) monitoring channel.
1.3. Invasive arterial pressure (IBP)
Invasive monitoring is the standard for patients with shock, severe hypotension, on vasopressor support or during mechanical ventilation.
The monitor must support:
Minimum 2 invasive channels
Pressure waveform display
SYS / DIA / MAP determination
Zero calibration (zeroing)
Ability to select pressure type (ART, CVP, PAP, ICP, etc.)
Signal stability and minimizing baseline drift are key.
1.4. Pulse oximetry and saturation (SpO₂)
Monitoring pulse oximetry parameters allows for real-time assessment of blood oxygenation.
Requirements for ICU:
Resistance to motion artifacts
Correct operation at low perfusion
Plethysmographic curve display
Pulse rate calculation
In patients on mechanical ventilation, pulse oximetry is used to assess the effectiveness of oxygenation.
1.5.Capnography
Monitoring of capnography parameters, in particular end-tidal CO₂ (EtCO₂), is mandatory in patients on mechanical ventilation.
The monitor should provide:
Display of the capnogram (CO₂ waveform)
Numerical value of EtCO₂
Measurement in mmHg, kPa or %
Compatible with sidestream (sidestream capnography) or mainstream (mainstream capnography) technology
Monitoring of capnography parameters allows to assess ventilation, perfusion and the effectiveness of cardiopulmonary resuscitation.
1.6. Temperature monitoring
In critically ill patients, temperature control has prognostic value (affects the diagnostic outcome).
The monitor must provide:
Minimum 2 channels
The ability to simultaneously monitor central and peripheral temperature
Display of temperature difference (ΔT)
1.7. Respiratory monitoring
In intensive care, the patient monitor must support:
Impedance control of respiratory rate
Apnoea alarms
Display of respiratory waveform graph
It is important that the algorithm is resistant to cardiogenic artifacts in patients with tachycardia.
The modular architecture in intensive care provides flexible formation of the monitoring configuration depending on the clinical condition of the patient and the profile of the department.
Structurally, the system consists of:
The basic monitor unit (screen, processor, control system),
Slots for installing measuring modules,
Separate replaceable modules with their own measuring boards and analog-to-digital converters.
2.1. Principle of distributed signal processing
In modular systems, the primary processing of biosignals is performed directly in the module. This reduces:
Level of electromagnetic interference
Influence of mutual channels
Data transmission delay
The digitized signal is transmitted to the monitor’s central processor for display, analysis and alarm generation.
2.2. Parameter configuration
Modular and the architecture allows for an individual configuration for each intensive care bed.
A typical intensive care configuration may include:
Multi-parameter module (block) (ECG, NIBP, SpO₂, Temp)
Invasive pressure module (2–4 IBP channels)
Capnography module (CO₂)
Anaesthetist gas detection module
BIS or extended EEG monitoring module
Adding a new parameter does not require replacing the base monitor - it is enough to install the appropriate module. For the intensive care unit, the ability to replace or add a module without interrupting the system is critically important. The modular architecture allows for adapting the configuration when changing clinical tasks (cardiac resuscitation, neuroresuscitation, postoperative ICU).
In the intensive care unit, the patient monitor is integrated into a single centralized surveillance system that provides full control of the patient's condition in real time.
3.1. Central Monitoring Station
The central monitoring station provides:
Simultaneous display of data from multiple monitors
Viewing graphs, waveforms in real time
Alarm control from all connected beds
Archiving trends and events
Access to patient history
In the ICU, this allows medical staff to:
Monitor patients from the operator's (workplace) medical staff
Respond promptly to critical events
Reduce the risk of missed alarms by indicators
The number of simultaneously connected patient beds is determined by the system architecture and network bandwidth.
3.2.Network Integration
The monitor must support connection to the hospital’s local area network (LAN) via Ethernet or secure Wi-Fi wireless protocols.
Required features:
Real-time data transmission to a central station
Time synchronization between devices
Data backup in case of temporary loss of connection
Integration with the hospital’s medical information system (HIS/EMR)
It is important that the system supports standardized data exchange protocols that ensure compatibility with other hospital information platforms.
3.3. Data archiving and storage
For the intensive care unit, the following are essential:
Long-term trend storage (24–120 hours or more),
Alarm event storage,
The ability to export data for clinical analysis.
This is especially important during critical case analysis, quality of care audits, and medical record management.
Conclusion
The choice of a patient monitor for the intensive care unit is determined not only by a list of parameters, but by a set of technical and clinical characteristics. Key aspects include:
Full control of vital signs (ECG, NIBP, IBP, saturation, temperature monitoring, capnography)
Support for advanced monitoring of patients on mechanical ventilation and in sedation
Modular architecture for adaptation to clinical needs and rapid replacement/expansion of equipment functionality
Integration with a central monitoring station and a medical information system for continuous monitoring and archiving of data
Ensuring continuity of the monitoring system
A comprehensive assessment of these characteristics allows for increased accuracy of clinical decisions, prompt response to critical events, and overall patient safety in intensive care units.